Pediatric Examination and Board Review (32 page)
Read Pediatric Examination and Board Review Online
Authors: Robert Daum,Jason Canel

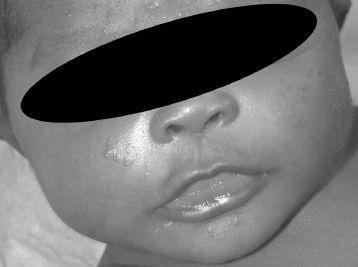
FIGURE 16-5.
See color plates.
ANSWERS
1.
(A)
This patient has a hemangioma. The description of the lesion becoming thicker and more nodular over the first couple of weeks of life is typical of the proliferative behavior of a hemangioma, as opposed to the stable nature of a port wine stain or other vascular malformations. Capillary malformation and port wine stain are synonymous. Angiosarcoma is a proliferative tumor, as is hemangioma. However it is extremely rare in newborns, whereas hemangiomas are present in up to 10% of 1-year-olds. Nevus sebaceous is classically located on the head, especially scalp, and is usually pebbly but not typically red in color or progressive as described.
2.
(E)
PHACES syndrome is the association of a large plaque-type facial
h
emangioma with
p
osterior fossa defects,
a
rterial defects,
c
ardiac defects,
e
ye abnormalities, and a
s
ternal raphe. Sturge-Weber syndrome is associated with facial port wine stains most often in the ophthalmic (V1) distribution of the trigeminal nerve; Klippel-Trenaunay syndrome is associated with port wine stains on the extremities and limb overgrowth. Neurofibromatosis and tuberous sclerosis are not typically associated with vascular birthmarks.
3.
(B)
An MRI of the head will identify the presence of a posterior fossa defect. It would also be an appropriate study to evaluate the presence of intracranial vascular malformations seen in Sturge-Weber syndrome. An echocardiogram might also be indicated to look for the cardiac features of PHACES syndrome; however, a good cardiac examination may obviate the need for an echocardiogram in all cases.
4.
(B)
The patient is experiencing early obstruction of the visual axis as a result of proliferation of the portion of the hemangioma involving the upper eyelid; therefore, intervention is indicated. Use of systemic corticosteroids is the best choice of the answers. It is beneficial in temporizing the growth and may expedite involution of hemangiomas during the active growth phase. It will also be critical to involve ophthalmology to follow this patient’s visual development. Laser therapy does not have a role in management of hemangiomas during the acute growth phase when the function of a critical structure is compromised. Laser cannot penetrate deeply enough into a hemangioma to decrease its bulk in most cases. Interferon alpha has been used in life-threatening hemangiomas, but the risk of irreversible spastic diplegia is a limitation.
5.
(C)
Hemangiomas undergo a proliferative growth phase during the first year of life. Subsequently they enter an involutional phase that may last up to 10 years or longer. Therefore, the flattening and fading observed occurs slowly and gradually over years. Port wine stains and other vascular malformations are stable, nonproliferative lesions and do not undergo involution. Surgical excision may be necessary ultimately to remove the residua of some hemangiomas, but in most cases it is best undertaken once a significant portion of the spontaneous involution has occurred. Some hemangiomas may leave superficial telangiectasias; these can be treated with laser therapy to decrease residual redness on the skin surface. Hemangiomas do not develop malignant neoplasms within them.
6.
(B)
A nevus sebaceous is a hamartoma of sebaceous glands typically seen in the scalp. They are hairless, slightly pebbly, and yellowish plaques in childhood, which may become more raised and nodular in adolescence. There is an increased risk of basal cell carcinoma developing in these lesions over the lifetime of the individual, typically not before young adulthood. Melanoma has not been associated with this lesion. Tinea capitis may cause hair loss, but generally there are also findings of scale, crust, broken hairs, and lymphadenopathy. Alopecia areata is a nonscarring form of alopecia that can occur at any age. Areas of hair loss are smooth without surface change. A nevus sebaceous is not typically associated with a risk for tethered spinal cord.
7.
(E)
A congenital nevus is a nevomelanocytic lesion present from birth. They are classified by size as small (0-1.5 cm), medium (1.5-19 cm), and large (≥20 cm). There is an increased risk of malignant melanoma in the large lesions, and these tumors have been reported in children before the age of 5 years. The medium and small lesions have a smaller risk of malignancy, and it is generally believed that this transformation rarely occurs before adolescence. Therefore, small and medium lesions may be observed for atypical changes or electively excised. Large congenital nevi are often technically difficult to excise. Laser procedures are not likely to remove all involved components of the lesion and therefore may not eliminate the risk of melanoma. There is no role for radiographic examination or cryotherapy.
8.
(A)
Solitary mastocytomas are not uncommon in infants. They appear as reddish brown plaques, sometimes with a slightly pebbled surface, and can become redder and more swollen with irritation, occasionally even blistering. As a diagnostic test, the lesion may be stroked firmly and observed for the reaction of redness and swelling; this is known as a Darier sign. Diascopy refers to applying pressure to a red lesion in an attempt to blanch it by temporarily clearing the intravascular blood locally. This technique is used to evaluate vascular lesions such as vasculitis and purpura. Transillumination and palpation for a thrill will not be revealing in the case of a mastocytoma. This history and examination are not suggestive of a cutaneous fungal infection; thus a scraping stained with KOH is unlikely to be helpful.
9.
(B)
Systemic antihistamines are useful in mast cell disease to decrease the symptoms associated with mast cell degranulation. Histamine is the prominent mast cell mediator, and degranulation of mast cell collections in the skin may occur spontaneously, with minor trauma or friction over a lesion, with environmental stimuli such as sudden heat or cold, and with many medications. Release of histamine causes lesions to become reddened, edematous, sometimes blistered, and often itchy. Use of systemic antihistamines can block or modify this response. Topical corticosteroids may be somewhat soothing but likely are not preventive. There is no role for permethrin or acyclovir in the management of mast cell disease. Excision might be curative for a single lesion but is not generally recommended.
10.
(C)
Urticaria pigmentosa is the condition of multiple cutaneous collections of mast cells that accumulate during infancy and childhood. The number of lesions can vary from few to innumerable. Childhood urticaria pigmentosa is rarely associated with systemic manifestations. Lesions tend to accumulate during the first few years of life, then stabilize, and gradually fade and involute by early adolescence. Some patients will have complete clearance; others will experience significant improvement. Adult-onset mast cell disease is associated with an increased risk of mast cell leukemia and other myelodysplasias; this has not been observed in the juvenile form.
 S
S
UGGESTED
R
EADING
Bruckner AL, Frieden IJ. Hemangiomas of infancy.
J Am Acad Dermatol.
2003;48:477-493.
Metry DW, Hebert AA. Benign cutaneous vascular tumors of infancy: when to worry, what to do.
Arch Dermatol.
2000;136(7):905-914.
Prose NS, Antaya RJ. Neoplastic and infiltrative diseases. In: Eichenfield LF, Frieden IJ, Esterly NB, eds.
Textbook of Neonatal Dermatology
. Philadelphia, PA: WB Saunders; 2001:442-444.
CASE 17: A NEONATE GIRL WITH VESICLES
A 5-day-old female infant is brought to the emergency department for evaluation of a rash. The child’s mother states that she has noticed small pus bumps developing on the infant’s face, body, and hands and feet. This is the first child of this young mother. She is also concerned because the child is spitting up her formula and sleeps a lot during the daytime but not at night. She is unsure whether the infant has had fever. She is also complaining of a new fever blister on her own lip.
On examination, pustules and vesicles are scattered on the chin, trunk, and palms and soles. Additionally, there are hyperpigmented macules and some areas of scaling at the edge of the macules. The child is afebrile, vigorous, and has moist lips and a wet diaper.
SELECT THE ONE BEST ANSWER
1.
A smear of a pustule is obtained and stained with Wright stain. Microscopic findings reveal
(A) sheets of eosinophils
(B) mites, feces, and ova
(C) multinucleated giant cells
(D) hyphae and spores
(E) sheets of neutrophils
2.
The best course of action is to
(A) perform a septic workup, including urinalysis, complete blood count (CBC), blood culture, and lumbar puncture
(B) admit the patient for intravenous (IV) antiviral therapy
(C) reassure the mother and discharge the patient home
(D) send a culture of the pustule fluid
(E) treat the infant with permethrin cream
3.
At this infant’s 1-month visit to the pediatrician, her mother is again concerned about a skin rash. She notes many red bumps on the face as well as a few pus bumps. She also is distressed by the many hyperpigmented marks on the trunk (
Figure 17-1
). The best management is
(A) hydrocortisone ointment to the rash twice daily
(B) benzoyl peroxide gel to the rash daily
(C) mupirocin ointment to the rash 3 times a day
(D) observation and reassurance
(E) ketoconazole cream to the rash daily