Resident Readiness General Surgery (59 page)
Read Resident Readiness General Surgery Online
Authors: Debra Klamen,Brian George,Alden Harken,Debra Darosa
Tags: #Medical, #Surgery, #General, #Test Preparation & Review

Less common causes include malignant hyperthermia and severe necrotizing wound infections.
POD 3: UTI, pneumonia, or anastomotic leak
POD 5: Deep venous thrombosis
POD 7 to 10: Intra-abdominal abscess
Basic initial workup of postoperative fever should include a CBC with differential, 2 sets of blood cultures, a urinalysis, and a chest x-ray. Additional studies such as CXR, sputum sample, venous duplex studies, or CT scan may be necessary in certain circumstances.
Acetaminophen (Tylenol) can be used to symptomatically treat fever. Downsides include suppression of the adaptive and normal physiologic response to infection, an inability to accurately follow a patient’s fever curve, and the possibility of hepatotoxicity.
COMPREHENSION QUESTIONS
1.
A 25-year-old female experiences a fever of 101.6°F on postoperative day 1 after a laparoscopic cholecystectomy. On evaluation, she looks and feels quite well. The most likely cause of her fever is which of the following?
A. Deep venous thrombosis
B. Urinary tract infection
C. Atelectasis
2.
All of the following are appropriate
immediate
first steps in the workup of a postoperative fever except which one?
A. Blood cultures
B. Abdominal CT scan
C. Urinalysis
D. Removal of the primary dressing
Answers
1.
C
. A fever on postoperative day 1 is most likely the result of atelectasis. This is even more likely in a patient who has undergone an operation that will result in diaphragmatic irritation and subsequent shallow breathing.
2.
B
. In most cases, the initial reflexive workup for a postoperative fever should include removal of the patient’s dressing to inspect the wound, 2 sets of blood cultures, and a urinalysis. Additional studies such as an abdominal CT should be obtained after discussion with a more senior member of the surgical team.
 A 42-year-old Woman 4 Hours Postoperative With a Fever and Extreme Pain
A 42-year-old Woman 4 Hours Postoperative With a Fever and Extreme Pain
Michael W. Wandling, MD and Mamta Swaroop, MD, FACS
You arrive at the bedside of a 42-year-old woman to perform a postoperative check four hours after she underwent a gastric bypass operation. Before you enter the room you note that she currently has a temperature of 102.3°F. She tells you her abdominal incision is excruciatingly painful, and on exam you are surprised by the unusual degree of tenderness in the region under and around her dressing.
1.
What is your next step?
NECROTIZING SOFT TISSUE INFECTION
Answer
1.
You should remove the dressing and examine the wound for any signs of necrotizing fasciitis.
The term necrotizing fasciitis was coined in 1951 to describe all gas-forming and non–gas-forming necrotizing infections, both of which shared the common feature of fascial necrosis. Recently, the term necrotizing soft tissue infection (NSTI) has replaced the older terminology, as this encompasses all infections regardless of the depth of tissue involved.
Patients who are most at risk for NSTIs include individuals with diabetes mellitus, obesity, peripheral vascular disease, chronic kidney disease, and alcohol abuse. NSTIs present with pain out of proportion to the physical exam, anxiety, and diaphoresis within 48 hours of bacterial inoculation in a wound. Other classic findings include erythema, pain or tenderness beyond the margins of erythema, woody edema, crepitus, bronzing of the skin, grayish, or “dishwater” discharge from the wound, skin necrosis, bullae formation, induration, fluctuance, fever, and hypotension. For examples of these skin findings, see
Figure 45-1
. Unfortunately, many of these distinctive features are late findings that are indicative of severe, life-threatening infection. You should therefore have a high index of suspicion for this type of infection, especially in a patient who has an otherwise unexplained fever in the acute postoperative period. In those cases it is incumbent on you to take down the dressing and, using sterile technique, examine the wound and surrounding skin.
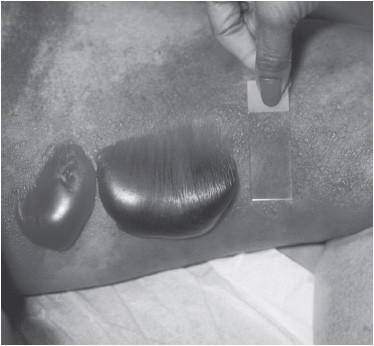
Figure 45-1.
Images of several examples of characteristic physical exam findings of NSTI. Variations in the appearance of bullae overlying NSTIs. (Reproduced with permission from Knoop K, Stack L, Storrow A, et al.
Atlas of Emergency Medicine
. 3rd ed. New York: McGraw-Hill Education; 2010. Figure 12.8. Photo contributed by Lawrence B. Stack, MD.)
Diagnosis
One of the hallmarks of NSTIs is a rapid progression of symptoms that can lead to death within hours. Delays in diagnosis and debridement are associated with a nine times greater mortality rate. It should be clear that any consult for a potential NSTI must be seen quickly, taken seriously, and be escalated to more senior residents or attendings should any suspicion of NSTI exist.
When evaluating a patient for an NSTI, it is essential to remember that the more dramatic physical exam findings associated with NSTIs are often not seen at the time of presentation, which can make differentiating them from nonnecrotizing infections difficult. Edema and erythema are almost always present, but are very nonspecific. You should at a minimum mark out the boundaries of the erythema in order to characterize the rate of spread of the infection.
While the physical exam can be nonspecific or even misleading, there are other features characteristic of NSTIs that can aid in making an early and potentially life-saving diagnosis. A basic set of labs can be key and should not be overlooked. A white blood cell count of >15,400 cells/mm
3
or a sodium level <135 mmol/L on admission to the hospital has an 80% positive predictive value and, if not present, an 80% negative predictive value, respectively, for NSTI.
